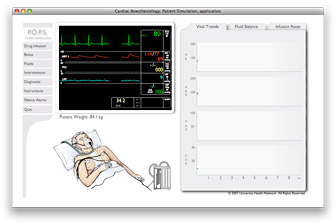
Post-operative intensive care
Note: This module was developed with Adobe Flash, and Flash is no longer supported by web browsers. However, there is a new Flash emulator called Ruffle which is under development. Currently, the POPS simulation is the only PIE Flash module that works with Ruffle, but as development is ongoing, future releases of Ruffle will work with other PIE modules. This will be indicated on the web page for each module.
Ruffle can be installed as an extension to the Chrome browser which will allow these modules to play. This extension can be downloaded from the Chrome Web Store:

Password
The entry of a Username and Password was for a project tracking user's scores which is no longer active. Please enter:
- Username: 1234
- Password: 1234
The challenge
This simulation covers post-operative care of a cardiac patient. Your patient has just been admitted to the Intensive Care Unit (ICU) following cardiac surgery. The surgical repair was successful, but the patient may have complications of depressed myocardial contractility, bleeding, hypo or hypertension, hypo or hypervolemia, hypo or hyperthermia, heart block, tamponade, and anemia.
Your task
Your task is to return the patient’s heart rate, arterial blood pressure, left atrial pressure, cardiac index and temperature to acceptable clinical levels and maintain patient stability within these levels for one hour of simulated patient time. In this simulation, time is speeded up by a factor of 60: one minute of real time is equivalent to an hour of time for the simulated patient. However, time stops while you are selecting your treatment options, so you have a chance to think about the intervention without further deterioration of the patient.
Interventions
You may treat the patient with the following interventions:
- Infusion medications
- Bolus medications
- Fluid replacement
- Warming or cooling the patient
- Cardiac pacing
- Return patient to OR for re-exploration for bleeding or relief of tamponade
Diagnostic information
- Vital signs from the patient monitor
- Visual indication of peripheral vasoconstriction
- Fluid intake and output
- Cardiac index
- Chest X-ray to check for tamponade.
Your score
You have one 12 hour shift to accomplish the task of initial patient stabilization and maintaining stability for an hour. For heart rate and vascular pressures, the monitor’s alarm limits define the limits of stability. Cardiac index should be maintained above 2.5 l/min/m2, and the temperature should be between 37 and 39oC. Your patient will be considered to do well and the simulation will end if you maintain ALL variables within these limits for 1 hour. The simulation will also terminate if the cardiac index remains below 2.5 l/min/m2 for 2 consecutive hours.